Mako Robotic partial knee resurfacing is a less invasive solution designed to restore the feeling of a natural knee.

Stefan D. Tarlow, MD, is an innovator; 9+ years ago he developed methods that transformed Mako Robotic Joint Replacement into an outpatient procedure.
In addition to his extensive experience with the more common medial unicompartmental knee resurfacing, he is one of the few Mako surgeons that has mastered lateral unicompartmental knee replacement surgery.
Each implant procedure is customized to precisely optimize your knee alignment, tracking and ligament tensioning. Mako Robotic partial knee resurfacing is a less invasive solution designed to restore the feeling of a natural knee.
PARTIAL KNEE RESURFACING WITH MAKOPLASTY®
The Mako Partial Knee application is a knee replacement treatment option designed to relieve the pain caused by joint degeneration due to osteoarthritis. Through CT-based 3D modeling of bone anatomy, surgeons can use the Mako System to create a personalized surgical plan and identify the implant size, orientation and alignment based on each patient’s unique anatomy. The Mako System also enables surgeons to virtually modify the surgical plan intra-operatively and assists the surgeon in executing bone resections.
SurgCenter of Greater Phoenix, an outpatient Joint Replacement Center in North Scottsdale cofounded by Dr. Tarlow, is an pioneer of Outpatient Joint Replacement. Stefan D. Tarlow, MD utilizes the MAKO robot technology in a surgical technique that resurfaces the damaged area of the knee without compromising the healthy bone, ligaments and tissue surrounding it. The robotic-arm assisted, minimally invasive procedure is performed through a small incision. In most cases there is a faster, less painful recovery than traditional joint replacement surgery. Many patients are back on their feet in just days. Consider this: the best surgical outcomes are in unicompartmental knee patients. Uni patients have a higher satisfaction score, lower chance of infection, stroke, heart attack, blood transfusion, blood clot and lower death rate compared to total knee replacement patients.
The process begins with a detailed evaluation, including an office visit with Dr. Tarlow for specific knee history, detailed physical exam and standing 4 view knee x-ray series. Usually, other special imaging tests are not required. After the decision to perform Mako is finalized, three main steps are completed to assure accurate sizing, precise implant alignment and proper balancing of the knee. Mako System surgery is an outpatient procedure with patients discharged to home from the Outpatient Surgery Center, alert and walking. Typical recovery includes using a cane or walker for a week and return to driving within 1-2 weeks. Most people return to work in 1-4 weeks. As a knee arthroplasty procedure (CPT 27446), MAKO Technology is typically covered by all health insurers. update 9/2022
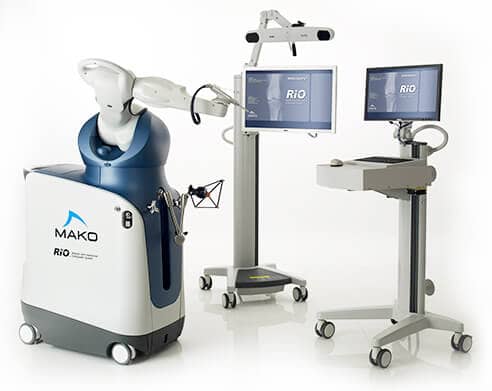
Mako is changing the way joint replacement surgeries are performed by providing each patient with a personalized surgical experience based on their specific diagnosis and anatomy. The virtual 3D model and the Mako Robotic System allows surgeons to create each patient’s surgical plan in the operating room. During surgery, the surgeon validates that plan and makes any necessary adjustments to optimize implant fit. The surgeon then guides the robotic-arm to execute that plan. Dr. Tarlow is an enthusiastic early adopter of this transformative technology.
Restoris MCK Partial Knee Implant System is the proprietary implant system designed for use with the Mako Robot for Partial (uni) Knee Replacement.
PARTIAL KNEE RESURFACING WITH MAKOPLASTY®

STEP 1
CT SCAN OF THE KNEE AT THE IMAGING FACILITIES
The CT provides precise, unique anatomic detail of your knee. This data is entered into the Makoplasty computer and is used both before and during the procedure to accurately plan implant size, orientation and alignment utilizing CT-derived 3-D modeling. A provisional sizing and positioning of components is done before surgical implantation.

STEP 2
INTRA OPERATIVE PLACEMENT OF COMPUTER NAVIGATION
This “tells” the computer in real time exactly where the knee bones are in space and provides kinematic detail about knee motion and knee ligament balance. This information is used to attain exact placement of the implant, still in the virtual realm at this point in time.

STEP 3
ROBOTIC ARM INTERACTIVE ORTHOPEDIC SYSTEM
The Robotic Arm Interactive Orthopedic System is now introduced into the knee using minimally invasive exposure and bone sparing removal of damaged tissue to form a shallow trough to allow the Restoris implants to be permanently placed into the knee, replicating the precise sizing and location derived from CT scan, Computer Navigation and virtual kinematics.
Commonly Identified Benefits of Robotic Knee Resurfacing:
WATCH RELATED VIDEOS
Ready to Schedule a Consultation?
Get started today by completing our request form. If you have additional questions, contact us by phone or e-mail, and our trained staff will assist you to the best of our ability or have Dr. Tarlow address your question when appropriate.
