Makoplasty Robotic Total Knee Replacement – An Innovation for Total Knee Replacement
ROBOTICS, MINIMALLY INVASIVE, CUTTING EDGE PROTOCOLS
Modern, state of the art Total Knee Replacement means Mako Robot planning and bone resection. Minimally invasive surgical exposure (Mid Vastus approach) combined with less traumatic tissue techniques minimize pain and swelling. Limited use of surgical tourniquet and bleeding prevention using TXA portend a quicker recovery and faster return back to a normal, active life. Robotic technology is is an integral part of this formula.
Dr. Tarlow is an innovation leader in robotic knee surgery. He is on the forefront, using the Mako Robot since 2011 for unicompartmental knee replacement. In November, 2016 Stefan D. Tarlow, M.D. was one of a select few of U.S. surgeons chosen for the long anticipated early clinical release of the Mako Robot for Total Knee Replacement. This surgery is typically performed as an outpatient procedure. The results over these 4 + years demonstrate improved patient recovery and more natural function vs. historical techniques.
Hear all about Mako Robotic Total Knee Replacement - Schedule a consultation with Dr. Tarlow to explore your options.
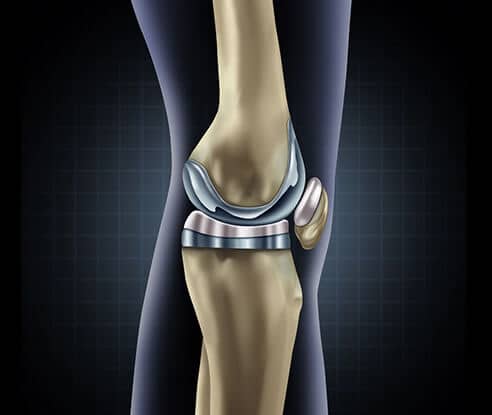
The Mako Robotic Total Knee application is a knee replacement treatment option designed to relieve the pain caused by joint degeneration due to osteoarthritis. Through CT-based 3D modeling of bone anatomy, surgeons can use the Mako System to create a personalized surgical plan and identify the implant size, orientation and alignment based on each patient’s unique anatomy. The Mako Robot System is utilized by the surgeon to perfect the surgical plan intra-operatively and the computer controlled robot precisely executes the bone resections. A cementless option, Triathlon Tritanium Cementless total knee system, became available for use with the Mako robot in 2017. For most patients, this is an option to consider. The implant for the standard cemented application using the Mako robot is the Triathlon Total Knee System. These implant systems are manufactured by Stryker Orthopaedics and are the proprietary implant systems designed for use with the Mako Robot for Total Knee Replacement.
In 2014 selected patients were discharged to home directly from the recovery room after Less Traumatic TKR. Our expertise has evolved. Outpatient Total Knee Replacement is a great option for most patients in 2020. Outpatient Total Knee replacement has advantages. Costs are lower since you are not paying to spend a night in a hospital bed and taking expensive hospital dispensed medications. Less over-treatment: less testing, less unnecessary procedures, and no medication errors can help avoid unwanted complications. Infections rates are lower when patients avoid hospital stays. The germs in your home are your friends because they live with you everyday. Hospital germs do not know you, can be nasty, and might cause harm.


Whether you choose Robotic or Traditional Total Knee Replacement the following fundamentals hold true:
Principles for Successful Total Knee Replacement:
- Multimodal Pain Control
- Bracing and Cryotherapy for Pain and Swelling Management
- Thirteen Step Infection Avoidance Protocol
- Bleeding Control with Pharmological Agent Tranexamic Acid
- Minimally Invasive Surgery: Smallest Workable Knee Incisions with Careful Handling of Knee Tissue
- Meticulous Surgical Attention to Detail for Proper Implant Sizing, Alignment, Rotation and Balancing
- Standardized Surgical Teams Improve Surgical Processes and Maximize Best Practices and Minimize Complications
- Home DVT prophylaxis with VenaPro sequential compression and oral Aspirin for 3 weeks duration
Is Traditional Total Knee Replacement or Mako Robotic Total Knee Replacement best for you ?
Mako Robotic (Less Traumatic) Total Knee Replacement
What I see in my day-to-day practice is mostly same day surgery with no hospital stay and quicker return to work/recreational activities for Less Traumatic Total Knee Replacement (MakoRobotic with Press Fit Stryker Triathlon implants is the go to method in 2019).
In 2019 healthy, motivated people go home the same day. These excellent outcomes are from advances in surgical technique including using the smallest workable knee incisions, careful handling of knee tissue, improved implant design ( Stryker Press Fit technology), multimodal pain management, thirteen step infection avoidance treatments, pharmacologic bleeding control, and improved rehabilitation methods (cold therapy, compression bracing, neuromuscular stimulation, early activity, and vit D/Essential AminoAcids). Standardized surgical teams improve surgical processes and maximize best practices and minimize complications.

LET OUR TEAM SHOW YOU HOW LESS TRAUMATIC TOTAL KNEE REPLACEMENT CAN IMPROVE YOUR LIFE.
KNEE ARTHRITIS TREATMENT OPTIONS
Advanced arthritis of the knee symptoms (pain, stiffness, limited motion, decreased walking and standing tolerance) often times intensify to the point of interfering with daily activities and causing intolerable pain during some or all activities. For these people, surgical intervention using knee joint replacement implants often times returns patients back into their normal life style with markedly diminished or no knee pain.
NON SURGICAL "STEP TREATMENT" ALTERNATIVES TO TOTAL KNEE REPLACEMENT
Self directed treatments can be helpful in cases of mild to moderate knee osteoarthritis. These measures includes optimizing body weight, daily aerobic low impact exercise, activity modification/rest, ice and OTC pills such as ibuprofen, naproxen, or acetaminophen. Physician directed treatments include physical therapy, prescription anti inflammatory NSAID like Celebrex or Mobic, Cortisone injections, Visco gel injections, arthritis unloader bracing, acupuncture, and if indicated for meniscal tear or loose body – knee arthroscopy.
TOTAL OR MAKOPLASTY PARTIAL REPLACEMENT - HOW TO DECIDE WHICH IS BEST?
Total Knee replacement is done when 2 or 3 of the knee compartments are completely worn out. These patients typically limp, have crooked legs (varus- bow leg or valgus- knock knee) and limited knee motion. Partial or Unicompartmental Knee replacement is done robotically using Mako technology when only one compartment is diseased or injured.
TOTAL KNEE IMPLANTS SYSTEMS?
The key for a successful Less Traumatic Total Knee Replacement is precise implantation by a skilled and experienced surgeon. Doctor Tarlow’s system of choice is the Stryker Triathlon Press Fit CR Knee for primary TKR (first time surgery). The Ortho Development Balanced Knee System is the revision system preferred by Dr. Tarlow.
PATIENT HEALTH OPTIMIZATION
Patient health optimization is key to a good surgical outcome. Patients should get 30 minutes of low impact, aerobic exercise (break a sweat) for at least 6 weeks prior to Knee Replacement surgery, even if it causes knee pain. Vitamin D and Essential Amino Acids may help your body heal. Patients should have a reasonable Body Mass Index (lower than 35 is good, 40 may be acceptable). A physician may help with weight loss. Smokers should refrain from smoking for 6 weeks prior to surgery and not smoke for the 2 months after their joint replacement. Help to stop smoking is available from ASHLINE. Diabetics, type 1 and 2, need to have Hemoglobin A1C less than 8 around the time of surgery and on the day of surgery blood sugar should be less than 150. Much higher risks for a bad outcome are associated with obesity, smoking and diabetes, with complications occurring at an unacceptable rate for patients with all three of these risk factors.The goal is to have a positive experience with Knee Replacement Surgery. The best course of action is to optimize your health to minimize complications..
Less Traumatic Total Knee Replacement
What I see in my day-to-day practice is that hospital stays are not required and return to work and recreational activities are excellent for Mako Robotic Total Knee Replacement patients. These good outcomes are from advances in surgical technique including using the smallest workable knee incisions with careful handling of knee tissue, MakoRoboticTechnique, Press Fit implant design, multimodal pain management, thirteen step infection avoidance treatments, pharmacologic bleeding control, and improved rehabilitation method(coldtherapy,compressionbracing,NeuroMuscularStimulation and earlyactivity).Standardized surgical teams improve surgical processes and maximize best practices and minimize complications.
MakoRobotic Total Knee Replacement patients routinely recover with less pain and have a faster return to normal function due to multimodal pain management, improved traditional surgical techniques, and rapid rehabilitation protocols.
I will continue to evolve surgical techniques and incorporate new technologies into the practice of orthopedic surgery to improve patient experience and patient outcomes.
The Current State of Affairs in Total Knee Replacement Surgery
Mako Robotic Total Knee Replacement surgery uses a robotic arm, 3-D virtual planning computer navigation and haptic guidance. Improvements over the last decade in traditional surgery techniques, multimodal pain management, infection prevention and rapid rehabilitation protocols produce the best patient recovery paths. Our patients do great!
Typical Recovery: Same Day Surgery. Walker/cane for 5-10 days. Driving within 1-2 weeks. Return to work in 1-3 months. Results vary depending on individual’s physical condition, other constitutional characteristics. Many patients take a year to reach a completely healed state. Typical Risks include infections, blood clots, wound bleeding and knee stiffness. Antibiotics are used in the pre-operatively to lower infection risk. Aspirin, Sequential Compression Devices and early mobilization are used to lower risk of blood clots. Aggressive, early Physical Therapy for 6-8 weeks is used to maximize range of motion and function.
Billing and Coding: The CPT billing code for TKR is 27447, for unicompartmental knee replacement 27446 and for patellofemoral arthroplasty 27438. These codes are useful to patients when discussing cost with insurance companies or surgeons. If you would like to know more or have specific questions about medical costs, email me.
Typical Risks include infections, blood clots, wound bleeding and knee stiffness. Antibiotics are used in the peri operative period to lower infection risk. Aspirin, Sequential Compression Devices and early mobilization are used to lower risk of blood clots. Aggressive, early Physical Therapy for 6-8 weeks is used to maximize range of motion and function.
ProPublica Surgeon Scorecard Data
Rating surgeons is still an inexact science. Dr. Tarlow chooses to include a link to his data so that patients are informed. Dr. Tarlow’s adjusted complication scale is in the best quartile. Of the 19 surgeons rated in Dr. Tarlow’s geographic area 14 surgeons had a greater and 4 surgeons had a lesser complication scale. That being said, the range of complication scale for our geographical area is 1.4% – 3.3%. I would opine that all surgeons in our area are performing well. Healthline analyzed data on over 1.5 million Medicare and privately insured people to take a closer look at these complications. Based on this analysis, 4.5 percent of patients under the age of 65 experience complications during this period. However, the same data set showed that the complication rate more than doubles for older adults ProPublica (Medicare data – patients 65 year or older) has a uniform rating system that compiles hospital derived data on 300 potential complications that can occur anytime within the first 30 days after Total Knee Replacement surgical procedures. These include procedure specific complications such as post op infection, blood clots and other complications such as heart attack, breathing problems or kidney failure. Since all orthopedic surgeons are rated using the same system there is some validity to adjusted complication scale. It is also important to state that a zero complication rate is not reality for major surgery such as total knee replacement.
Guidelines for Antibiotics After Total Knee Replacement
In 2016 this recommendation was published by the AAOS and a clinical practice guideline was published: In 2020 to increase utilization and ease of use the content from the AUC has been converted to an at-a-glance decision tree highlighting the key takeaways (decision tree below) Current recommendation is ANTIBIOTICS are not required if healthy patient without dental infection. Susceptible patients (diabetes, HIV, Rheumatoid on immunosuppresive meds, Cancer patients immunocompromised – to name a few) and patients with a previously infected total joint replacement should always use prophylactic antibiotics for Dental work.
If antibiotic prophylaxis is desired the dosing is as follows.
For dental prophylaxis, one dose Amoxicillin 2 grams orally one hour prior to dental work is standard.
Use Clindamyacin 600 mg if PCN allergic.

WATCH RELATED VIDEOS
Makoplasty Robotic Assisted Knee Surgery Videos
Ready to Schedule a Consultation?
Get started today by completing our request form. If you have additional questions, contact us by phone or e-mail, and our trained staff will assist you to the best of our ability or have Dr. Tarlow address your question when appropriate.


