Knee arthroscopy is one of the most common orthopedic surgeries performed at hospitals and outpatient surgical centers.
Knee arthroscopy is one of the most common orthopedic surgeries performed at hospitals and outpatient surgical centers. General anaesthesia is administered to patients undergoing the procedure. A thin telescope with a fiber optic light cable attached to its side port is one of the tools used in the procedure. The telescope also has an HD video camera on the optic eyepiece. The device is inserted into the knee to cut torn flaps of meniscus, remove loose tissue, or press rough joints. Doctors also inject a sterile saline fluid into the knee joint to get a clear view of the knee capsule.
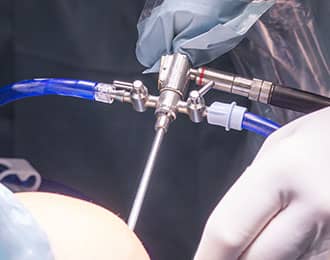
The surgery takes about 30 to 45 minutes, and patients can go home an hour or two after the procedure. Patients may need to use crutches and take oral pain medications for a week. They may return to work in two to four days after the procedure, but must not overstress their bodies. Full recovery period may last for about two to four weeks. This is recommended for menisectomy, chrondroplasty, lateral release, and loose body removal surgeries.
Results for knee arthroscopy may depend on the patient’s age and diagnosis. Patients below 50 years of age with only one knee problem (i.e. loose body, small joint surface damage, and torn meniscus) often have higher success and recovery rates after the surgery. Some patients who are above the standard treatment age and have multiple conditions may experience less predictable outcomes following the procedure.
ARTHROSCOPIC KNEE SURGERIES
DIAGNOSTIC ARTHROSCOPY
Even with high-resolution 3T MRI scans, Orthopedic Surgeons may need to utilize direct visualization of the knee joint to correctly diagnose a knee condition. Specialists conduct diagnostic arthroscopy prior to or at the time of meniscal repair, Autologous Chondrocyte implantation, microfracture procedure, evaluation of arthritis, or assessment of ligament injury.
In some cases the knee diagnosis is uncertain even after a detailed history, physical exam, X-ray, and MRI. Diagnostic arthroscopy may help with discovery of the correct diagnosis in cases of unexplained knee symptoms.
ARTHROSCOPY MENISECTOMY
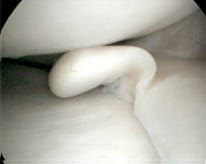
This procedure removes the torn meniscus (and leaves the healthy meniscal tissue in the knee) which alleviates symptoms such as swelling, locking, or pain. Doctors often recommend this surgery for patients who are 25 to 55 years old, as the knees and articular cartilage are still in their prime condition. [above photo shows flap tear of medial meniscus with healthy articular cartilage – this case will result in surgical cure for the patient].

ARTHROSCOPIC MENISCAL REPAIR
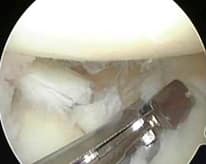
This procedure involves inserting meniscal sutures or anchors to hold the torn meniscus for natural healing. This technique is only utilized when the tear pattern of the meniscus is at the periphery and the body of the meniscus is uninjured. The blood vessels in the meniscus allow the meniscus to heal. This tear pattern is less common, but when it is present meniscal repair is a good option and restores the knee back to normal for Arizona patients. (see above arthroscopic photo).

ARTHROSCOPIC CHONDROPLASTY/MICROFRACTURE
Chondroplasty refers to a technique in which an arthroscopy shaver blade is used to smooth the rough edges and remove the loose articular cartilage (joint surface) around a defect in the articular cartilage. Results are highly variable. Microfracture (see above knee cartoon) describes a technique in which the surgeon uses an ice pick-like tool to penetrate the bone surface just under the articular cartilage in a defect where articular cartilage has died and flaked off the underlying bone. The principle is based on the idea that the marrow element cells released by this “micro fracturing” will fill the joint surface defect and mature into tissue to replace the lost cells. This works best when the defect is less than 2 centimeters in diameter and the patient is less than 30 years of age. Special post op care is mandatory for a good outcome and return to sports can be many months.

ARTHROSCOPIC LATERAL RELEASE
This is an arthroscopic treatment of patellar tracking abnormalities, specifically lateral patellofemoral compression syndrome, with or without associated patellar joint surface injury. The surgeon will use thermal or cautery to arthroscopically cut through the lateral retinaculum (depicted in black in the above diagram, red line is the cut in the retinaculum) in order to release the tension on the tissue. In theory this will allow your patella to return to a normal position. Success is 50 %.

ARTHROSCOPIC LOOSE BODY REMOVAL
Loose pieces of bone or articular cartilage or composite of both can break loose and float in the knee, causing symptoms of pain, locking and catching. Most commonly loose bodies are seen in older patients when bone spurs break off the margins of the knee joint. In younger patients loose bodies are the result of patellar (knee cap) dislocation, shear or direct blow injury, and osteochondritis dissecans. Arthroscopic loose body removal is a predictable and helpful procedure for patients. Recovery is usually quick.
WATCH RELATED VIDEOS
Makoplasty Robotic Assisted Knee Surgery Videos
Ready to Schedule a Consultation?
Get started today by completing our request form. If you have additional questions, contact us by phone or e-mail, and our trained staff will assist you to the best of our ability or have Dr. Tarlow address your question when appropriate.
