PRP (platelet rich plasma) is an injection treatment performed in the office. PRP for the knee is a biologic regenerative medicine treatment that does not require a surgical procedure.

Dr. Tarlow injects PRP directly into the diseased site which may stimulate a regenerative repair process.
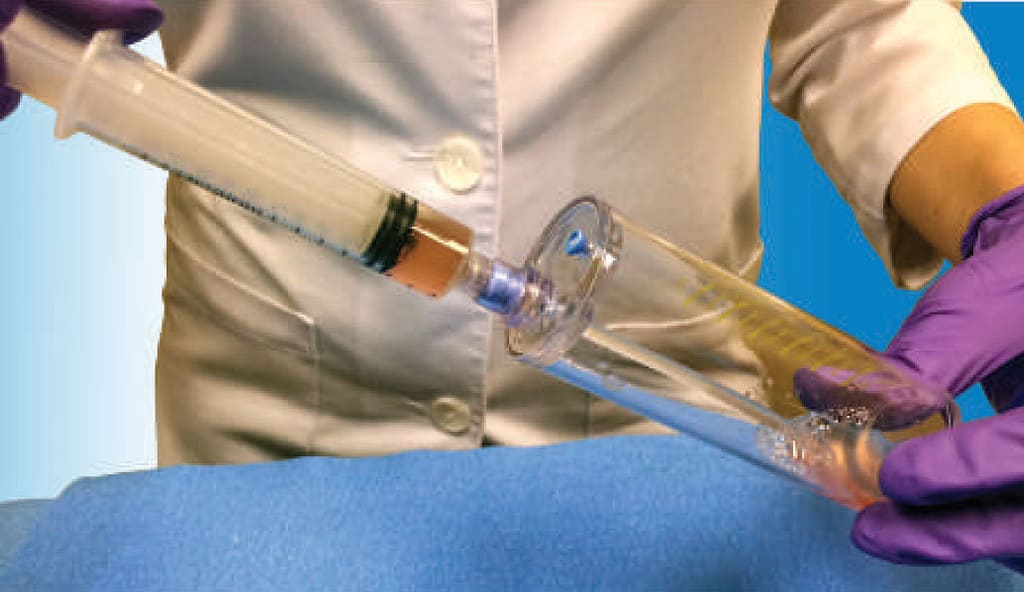
PRP comes from your blood. A nurse draws the needed amount from your arm which is then processed in the office. The PRP produced is then injected into your knee. The process takes 1 hour. The preparation we use is Emcyte PurePRP.
PRP FOR CHONDRAL DEFECTS: PARTIAL THICKNESS KNEE LESIONS
Knee chondral defects have a limited capacity for self-repair due to the low biologic activity of chondrocytes and its lack of blood supply. Articular cartilage defects often fail to heal spontaneously. Partial chondral defects untreated are a source of chronic knee pain and knee swelling.
PRP is used to treat the symptoms from partial thickness chondral defects of the knee. Platelet-rich plasma (PRP), with a rich source of autologous growth factors, can promote healing of partial thickness chondral defects in otherwise healthy knees. Platelets are involved in the complex process of tissue repair by the release of these growth factors. Studies have suggested that PRP stimulate either cell proliferation or matrix metabolism by articular chondrocytes.
PRP FOR OA (OSTEOARTHRITIS KNEES)

This treatment is used to modify the symptoms of knee OA (osteoarthritis) by counteracting the natural process of Osteoarthritis which alters the normal joint metabolism resulting in increased cell breakdown and decreased cell repair.
PRP is used to treat the symptoms from mild to moderate OA of the knee. Platelet-rich plasma (PRP) can mitigate the symptoms of pain and swelling from knee OA by modulating the inflammatory process. This acts to promote healing and suppresses the inflammation that causes knee pain.
HOW DOES IT WORK IN OA & CHONDRAL DEFECT KNEES?
In the knee, the release of growth factors from PRP occurs immediately and lasts for around three weeks and the clinical effect tends to wane down by the end of the year. Prolonged and sustained release of growth factors from platelets could possibly help in biological healing and anti-inflammatory effects.
More specifically (and a bit technical):
PRP acts at various levels to alter and improve the joint homeostasis.
Within the knee: Platelet alpha-granules contain and release numerous growth factors, including hepatocyte growth factor (HGF), vascular endothelial growth factor (VEGF), platelet-derived growth factor (PDGF) and transforming growth factor-b (TGF-b) , which are good proteins in may promote healing.
The cells lining the knee, synoviocytes are influenced by increased hyaluronic acid (HA) secretion, creating a more favorable and balanced state of blood flow, and a decreased of "bad proteins" like interleukin-1 (IL-1) and matrix metalloproteinases (MMPs).
An overall suppression of the joint inflammation can explain the pain reduction effect, which is the most prominent and disabling symptom of knee OA.
Ready to Schedule a Consultation?
Get started today by completing our request form. If you have additional questions, contact us by phone or e-mail, and our trained staff will assist you to the best of our ability or have Dr. Tarlow address your question when appropriate.
