This video guides you through to airport check point process.
Open this link to print an optional TSA notification card to carry with you at the airport checkpoint.
Knee Surgeon and Specialist Stefan D. Tarlow, M.D.
This video guides you through to airport check point process.
Open this link to print an optional TSA notification card to carry with you at the airport checkpoint.
What works:
Strengthening Exercises with neuromuscular education*
NSAID (pills such as ibuprofen and naproxen)
Appropriate weight loss if BMI > 25
Total or partial Knee Replacement
Cannot Recommend for or against:
IA steroid injection
Acetaminophen
Manual therapy, electrotherapeutics
Knee arthroscopy for meniscus
Cannot Recommend:
IA Hyaluronic Acid (viscosupplementation)
Braces
Arthroscopy – clean out
Glucosamine and Chondroitin
Acupuncture
Insoles
*The Alexander Technique (AT) is a method of neuromuscular re-education which aims to teach individuals how to improve postural support, reduce potentially harmful patterns of muscle tension and improve control of response. AT lessons provide an individualised approach to developing skills that help people recognise, understand, and avoid poor habits adversely affecting postural tone and neuromuscular coordination.
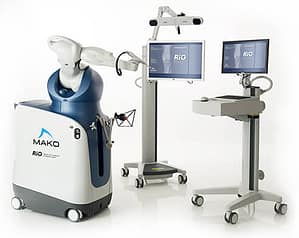 Dr. Tarlow utilizes the world’s most advanced orthopedic robotic arm and computer software system at HonorHealth’s Scottsdale Healthcare Thompson Peak. Each implant is customized to precisely optimize your knee alignment, tracking, and ligament tensioning to extend the life of your implant. Makoplasty Robotic partial knee resurfacing is a less invasive solution designed to restore the feeling of a natural knee. Every patient is unique. Every result is precisely beautiful. Walk away from your knee pain today!
Dr. Tarlow utilizes the world’s most advanced orthopedic robotic arm and computer software system at HonorHealth’s Scottsdale Healthcare Thompson Peak. Each implant is customized to precisely optimize your knee alignment, tracking, and ligament tensioning to extend the life of your implant. Makoplasty Robotic partial knee resurfacing is a less invasive solution designed to restore the feeling of a natural knee. Every patient is unique. Every result is precisely beautiful. Walk away from your knee pain today!
Advanced Knee Care, P.C. and Scottsdale Healthcare Thompson Peak is one of a few locations worldwide to offer partial knee resurfacing with MAKOplasty®, a technique that resurfaces the damaged area of the knee without compromising the healthy bone, ligaments and tissue surrounding it. The robotic-arm assisted, minimally invasive procedure may offer a smaller incision and a faster, less painful recovery than traditional joint replacement surgery, with many patients back on their feet in just days.
The process begins with a detailed evaluation including an office visit with Dr. Tarlow for specific knee history, detailed physical exam and standing 4 view knee x-ray series. Other special imaging tests might be required. After the decision to perform Makoplasty is finalized, three main steps are completed to assure accurate sizing, precise implant alignment, and proper balancing of the knee.
Step One: CT Scan of the knee done at Scottsdale Healthcare Thompson Peak (must be done at this facility – CT machine is specifically calibrated for Makoplasty procedure). The CT provides precise, unique anatomic detail of your knee. This data is entered into the Makoplasty computer and is used both before and during the procedure to accurately plan implant size, orientation and alignment utilizing CT-derived 3-D modeling. A provisional sizing and positioning of components is done before surgical implantation.
Step Two: Intra operative placement of Computer Navigation. This “tells the computer” exactly where the knee bones are in space and provides kinematic detail about knee motion and balance. This information is used to refine exact placement of the implant, still in the virtual realm at this point in time.
Step Three: Integration of step one and two allow precise virtual placement of the implant through real-time intra-operative adjustments for correct knee kinematics and soft-tissue balance.
Makoplasty is an inpatient procedure with a usual one-night hospital stay. Typical recovery includes using a walker for a week and return to driving within 2 weeks. As a knee arthroplasty procedure, MAKOplasty® is typically covered by most health insurers.
The Robotic Arm Interactive Orthopedic System is now introduced into the knee using
minimally invasive exposure and bone sparing removal of damaged tissue to form a shallow trough to allow the Restoris implants to be permanently placed into the knee replicating the precise sizing and location derived from CT scan, Computer Navigation, and virtual kinematics. RIO® assists the surgeon in achieving natural knee kinematics and optimal results at a level of precision previously unattainable with conventional instrumentation.
Implant Design, Surgeon Experience, and Patient Age greater than 65 years are associated with improved outcomes for unicompartmental knee replacement. This is sometimes termed Makoplasty or partial knee replacement. In Dr. Tarlow’s opinion, precise implant placement using computer navigation and virtual modeling and robotic arm guided resection will be shown further improve outcomes.
Unicompartmental Knee arthroplasty (ZUKA) had a 1 % revision rate, the Oxford Mobile Bearing 1.7 % revision rate and all others tested were 6 % or greater. The Restoris implant used for Makoplasty incorporates all the important design characteristics of the ZUKA implant.

Usually, osteoarthritis of the Knee involves the entire joint, and a Total Knee Replacement is the treatment of choice. Perhaps one in ten people with knee osteoarthritis with severe enough involvement of the joint to consider surgery are fortunate enough to have the arthritis limited to only one compartment of the knee. In this case Makoplasty partial knee replacement is the best surgical choice. The knee has 3 compartments (think of the knee as a 3 room home). When just one compartment has all the articular cartilage or joint surface damaged (one bad room, two good room) partial knee replacement is done. This is also known as unicompartmental knee replacement (uni) if the medial or lateral compartment between the femur and tibia (thigh and shin bone) is replaced or patellofemoral replacement if the joint between the femur and patella (thigh and knee cap bone) is replaced.
Unicompartmental knee replacements function better than total knee replacements because less of the normal anatomy is disturbed ( no knee ligaments removed, less bone removed) and the uni knee bends, straightens and rotates more naturally. Recover after unicompartmental knee replacement is quicker and the postoperative pain is less compared to total knee replacement.
Longevity of a unicompartmental knee is very good, with nine in ten uni’s working well at 10 years after surgery and many functioning well 20 years after surgery. The most common cause of failure after uni knee replacement is advancing arthritis in one or both of the previously uninvolved compartments of the knee.
Here is an excerpt of an article in the Arizona Republic about one of my patients in whom I performed partial knee replacement in one knee, then 3 months later the other knee. This is an example of how well partial knee replacements function. Outcomes like this is why I wanted to practice medicine.
“After suffering for years with knee damage that limited her mobility, Sarah Panepinto does not take dancing with her husband or playing tag with her kids for granted.
Last year, the 41-year-old Gilbert mother of five children had partial knee-replacement surgery on both of her knees. Since then, Panepinto said her recovery has been a miracle.
I can dance. I’m speed-walking. And I can even play Dance, Dance, Revolution with my kids,” Panepinto said.
The more active lifestyle is a blessing for Panepinto who needs the energy to keep up with the home-schooling of her two teens and two elementary school-age kids.
I’m off anti-depressants . . . I feel like I have my life back,” said Panepinto who has suffered from knee problems since she was 12.”
20 year survival rates of unicompartmental knee replacement approach 75 % or better. Implant design and Makoplasty surgical technique (robot technology) are important contributing factors.
Berlin surgeons performed a medical study evaluating 5 year survival of German patients from 2006 to 2012. This was published in the JBJS in October of 2016.
Risk factors associated with failure of the implant in the first 5 years after implantation are:
1. age younger than 55
2. Obesity (BMI > 30)
3. Diabetes, complicated
4. Depression
5. Low volume facility (less than 10 cases per year)

Scottsdale Knee Specialist & Surgeon – Stefan D. Tarlow M.D
Stefan D. Tarlow, MD, is Arizona’s premier “knees only” orthopedic surgeon.
more about us »
© 2024 | ALL RIGHTS RESERVED. ADVANCED KNEE CARE, STEFAN D. TARLOW, M.D.